
As the COVID-19 virus began to grip the United States, there was much uncertainty as to how fast the virus would spread, how severe the cases might be, and how highly contagious patients would impact access to hospital beds, ventilators, staffing, and PPE. For healthcare organizations, this situation led to growing concerns about operational protocols, particularly regarding the need for surge capacity to meet peak bed demand.
These concerns are not abating—COVID-positive cases are, in fact, increasing across the country, compounding annual demands from flu season, extending capacity constraints, and creating operational challenges and financial pressures.
Keck Medicine of USC, a 619-bed academic health system based in Los Angeles, 需要帮助确定第一波COVID-19患者可能如何影响其医院,并与ECG联系以开发预测模型. Working with Keck leadership, ECG预测了COVID-19在洛杉矶县的传播,并跟踪了该地区和凯克的两家普通急性医院——南加州大学凯克医院(KH)和南加州大学Verdugo Hills医院(VHH)的总床位需求。. 这种建模有助于凯克在重症监护中为covid -19阳性和covid -19阴性患者制定计划, medical-surgical, and pediatric units. Importantly, 它还帮助凯克确定在全州范围内推迟选择性程序后,何时以及如何增加非必要程序.
I. Modeling the Anticipated Impact of a Virus
Due to the nature of a novel virus and the lack of documented study of COVID-19, 目前尚不清楚哪种传染病模型能够最恰当地捕捉病毒的行为并进行充分的预测. ECG chose to use the susceptible, infectious, and recovered (SIR) model, a proven, differential equation model that groups the population into three compartments—S, I, and R—representing a set of dependent variables that are a function of time. SIR模型的好处之一是,它对病毒的不确定方面需要较少的假设, 例如,无症状患者是否具有传染性,以及患者在康复后能保持多长时间的免疫力.
ECG和Keck与洛杉矶县公共卫生部门合作,作为四个月期间每日感染计数的来源, utilizing the available data arranged by age cohorts. 该模型是用这些数据以及最新可用的人口普查数据构建和填充的.
Typically in modeling disease spread, the input assumptions are fairly well tested and studied; but due to the nature of the novel coronavirus, broader assumptions were required for the model’s other inputs, including the average contagious period; the R0, or transmission rate, which varies and changes based on a population’s behavior; and the comprehensiveness of testing. The model was structured to yield conservative, moderate, and aggressive scenarios to provide a range of outputs. 数据趋势被捕获,因此预测可以很容易地与历史信息更新.
图1是为说明COVID-19在洛杉矶县的传播而创建的图表之一.
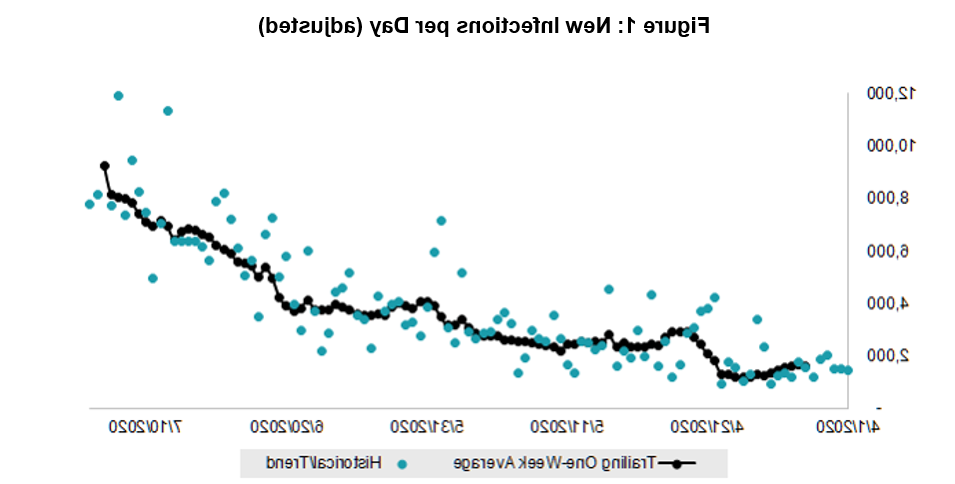
注:每日新增感染调整假设仅报告35%的新病例, 一个内置于模型中的变量,它会随着时间的推移根据各种因素进行修改.
II. Bed Demand
To determine overall bed demand for the county, 我们对全县可用床位总数和所需的非covid -19相关床位数量进行了建模. As a baseline for these totals, 我们采用了加州全州健康规划和发展办公室(OSHPD)对所有洛杉矶县普通急症护理医院的利用和财务数据. Although this data lagged current conditions, it proved to be the most applicable and readily available.
综合数据显示的是COVID-19对与COVID-19无关的患者数量的影响. 选择性手术被取消,病人们避开急诊科,, baseline hospital bed utilization was shrinking. 根据凯克的实际经验,他们对全国范围内预计的数量减少程度进行了假设,并定期进行了修改和更新. 基线需求减少与可用床位数量之间的差距代表了covid -19阳性患者的可用能力.
Figure 2 illustrates bed demand in Los Angeles County. 这表明,由于急诊科就诊和选择性手术减少,5月份床位需求出现了平静,然后随着病毒继续传播,需求从6月份开始再次增加.
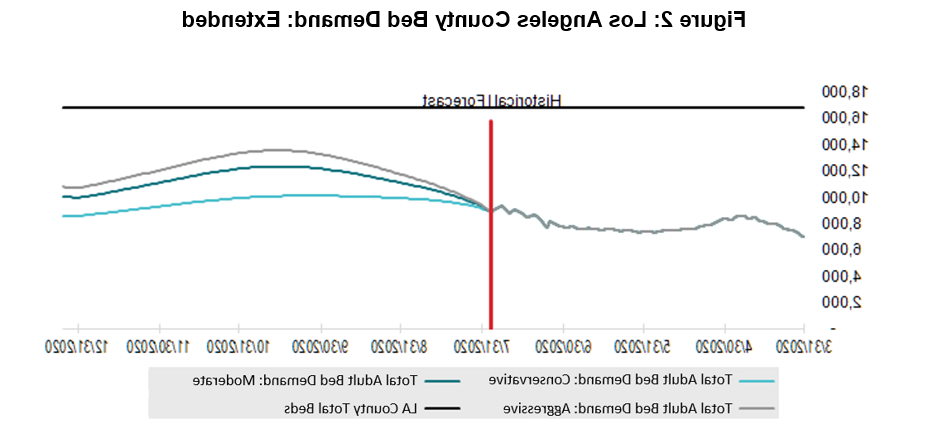
有了预测床位可用性和任何一天感染COVID-19的人数的模型, the number of infections could be translated into hospitalizations. This is where age cohort data enabled a more precise prediction, as the elderly were much more susceptible to the virus than younger people. Accordingly, hospitalization rates were assumed, including the proportion of hospitalizations requiring an ICU bed, based on the age group sensitivity and tracked data historically, making adjustments over time. We also made assumptions for hospital lengths of stay, sensitive to each age cohort and corresponding bed type, 以了解住院患者的COVID-19数量如何随着时间的推移而增加.
图3显示了根据医院非covid -19相关ICU人口和病毒传播对KH的影响,预计KH ICU床位需求. Despite KH’s lack of an ED, 在许多其他医疗机构中,哪一个是COVID-19患者的“前门”, a COVID-19 bed demand was observed and carefully managed via patient transfers.
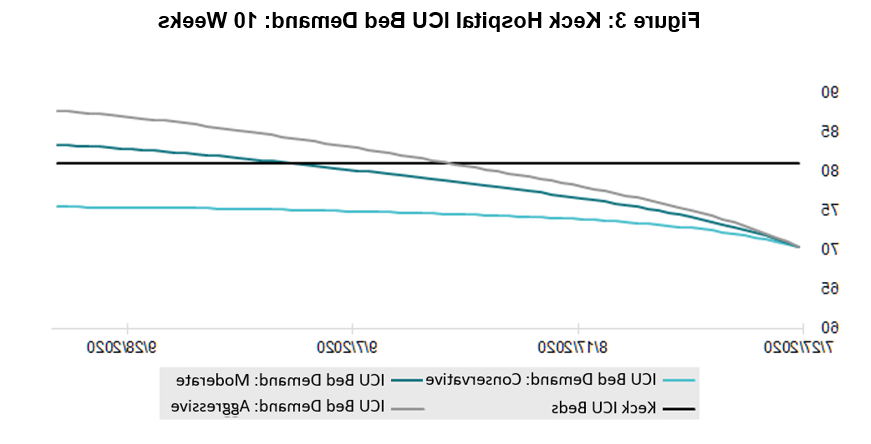
III. Conclusions and Expansion Possibilities
The model was updated and monitored daily from April through early August 2020, 当病毒的传播速度放缓到足以缓解按类型划分的床位容量方面的运营担忧时——至少在撰写本文时是这样. Fortunately, 到2020年10月,2019冠状病毒病导致的床位需求没有超过洛杉矶县的床位供应, nor at KH or VHH. 每家医院都建立了COVID-19床位单位,但不需要新建床位或临时床位来满足需求. This is changing, however, as the anticipated surge in cases has been realized, with increasing positive cases and hospitalizations across 41 of the 50 states
Ultimately, 通过建模练习获得的洞察力——由对模型的警惕维护推动——使凯克能够负责任地回到更高的入住率, with greater confidence, and over an accelerated time frame. 凯克能够系统地增加选择性程序,以帮助减轻其在大流行高峰期经历的财务压力(当时大多数医院都很常见)。. Should a second wave of COVID-19 or another pandemic be encountered, 这种模式可以为凯克医院重新启用,也可以类似地适用于全国任何其他医院或bet8网站备用.
At the time of this publication, 目前还没有公开的疫苗,目前的理解是,被感染的人可能在几个月后再次感染. COVID-19免疫力在几个月内减弱的可能性可能表明SIRS (i.e., susceptible, infected, recovered, 在较长一段时间内,易受影响的模型可能是一个更准确的预测工具.
With the upswing in COVID-19 cases and the advent of flu season, 与ECG联系,了解我们如何帮助您的组织更好地预测床位需求和资源部署.
Contact UsPublished November 4, 2020